KEY CONCEPTS
•
Carbon dioxide concentration in an indoor environment is not difficult to measure and provides an indication of potential exposure to COVID-19.
•
A model has been produced that provides an indication of the degree of risk of COVID-19 infection in a specific indoor environment by monitoring the level of carbon dioxide due to human exhalation.
•
The tolerable excess carbon dioxide level was determined in a classroom and found to be lower for individuals who are vocalizing and exercising.
The COVID-19 pandemic, as of the writing of this article, has been ongoing for more than 18 months since the beginning of 2020. During this time, there has been a considerable loss of human life, and many individuals who contracted the disease are still facing chronic health problems.
As noted in a previous TLT article
1 that discussed an STLE Webinar presented on how to safely get through the COVID-19 pandemic, the main mode of transmission for the virus causing this disease (SARS-CoV-2) is either through inhalation or ingestion. A key factor is that the size of virus particles can range from 60 to 140 nanometers and can remain in a specific indoor environment for hours.
Another factor to consider
(as shown in Figure 2) is the consideration that particle size plays an important role in transmission. Smaller viral particles have a better chance of moving further across an indoor environment than larger particles.
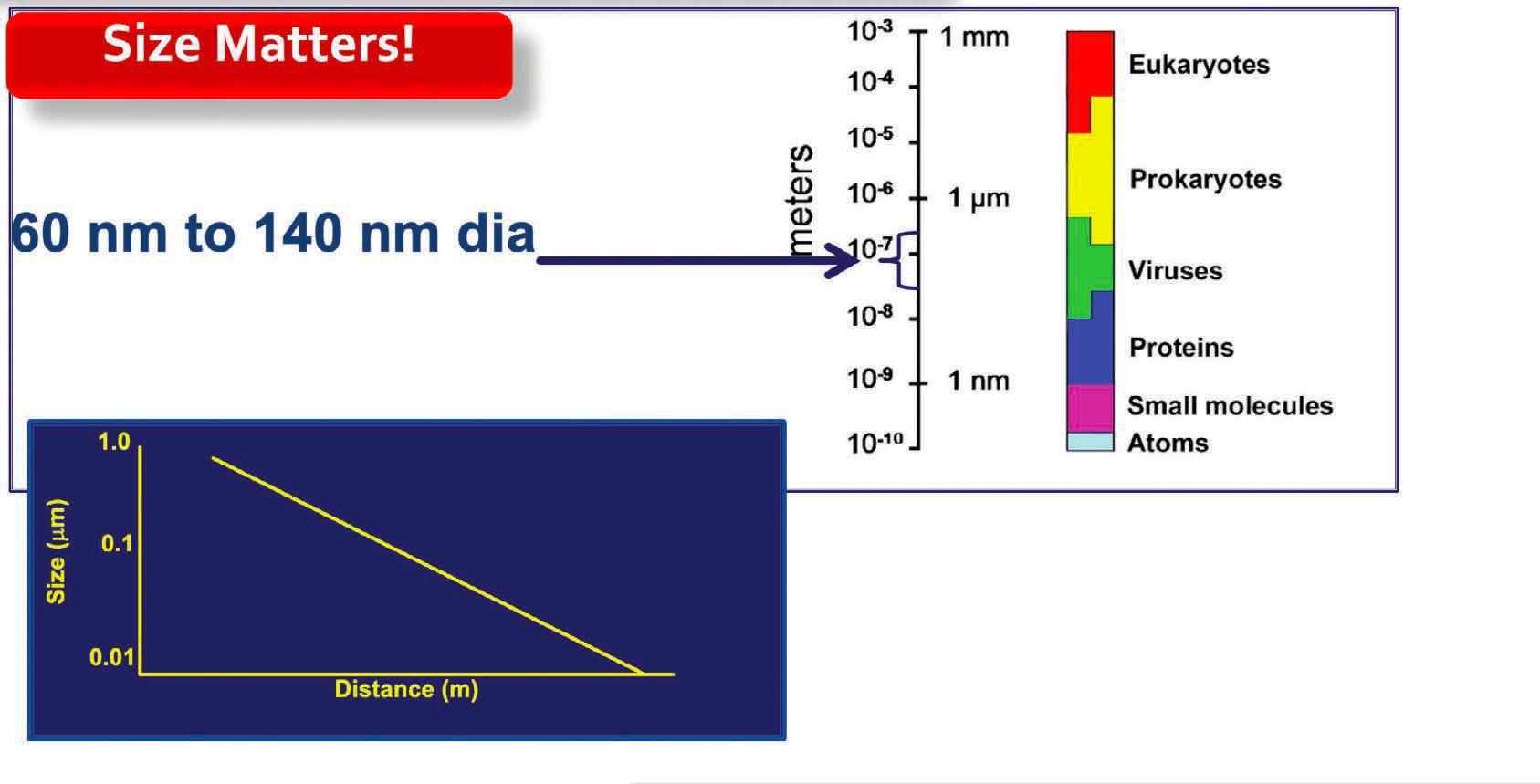 Figure 2. The small aerosol particles produced when COVID-19 is transmitted by an infected person have a better chance of moving further across an indoor environment than larger particles. Figure courtesy of STLE.
Figure 2. The small aerosol particles produced when COVID-19 is transmitted by an infected person have a better chance of moving further across an indoor environment than larger particles. Figure courtesy of STLE.
Dr. Zhe Peng, research scientist at the Cooperative Institute for Research in Environmental Sciences (CIRES) and in the department of chemistry at the University of Colorado in Boulder, Colo., says, “Ongoing research studying the transmission mechanisms for COVID-19 is concluding that the key mechanism for how this disease is spreading through the virus-containing aerosols is in the environment.”
This leads to the question about how to measure the concentration of SARS-CoV-2 viral particles. Peng indicates that direct measurement of virus containing aerosols is very challenging. An alternative is to monitor the concentration of carbon dioxide. The reasoning is that an individual infected with COVID-19 will exhale not only SARS-CoV-2 particles but also carbon dioxide.
Analysis of carbon dioxide levels in an indoor environment is not difficult and can be done with low-cost sensors. Peng adds, “The idea of measuring carbon dioxide levels as a strategy for determining the relative risk of becoming infected with COVID-19 is not new. Researchers proposed this approach about 20 years ago to monitor for the risk of catching the common viral disease, influenza.”
The primary source for carbon dioxide levels in an indoor environment is human exhalation. Peng says, “In most cases, the excess carbon dioxide concentration above background levels is due to the presence of individuals. Background levels of carbon dioxide originate outside of the indoor environment.”
Monitoring carbon dioxide as a means for determining the infection risk of COVID-19 can prove to be effective not just in a home environment but also in an office or laboratory. Peng says, “Determination of carbon dioxide in a manufacturing environment is more complicated because of the possible presence of combustion sources that generate more carbon dioxide than what comes from exhalation.”
Past studies attempted to propose a single carbon dioxide threshold concentration that must be met to indicate a high degree of risk. With differences in the types of indoor environments and activities, an attempt to come up with a simplified solution is not accurate and can be misleading.
A new study has now been completed to produce a model that can provide an indication of the degree of risk of COVID-19 infection in a specific indoor environment.
Infection risk analysis for various environments
Peng and his colleague Jose-Luis Jimenez, CIRES Fellow and professor in the department of chemistry at the University of Colorado, developed a zero-dimensional (box) model to study various scenarios where individuals will gather in indoor environments. Peng says, “As part of our modeling, we assumed that the air is well-mixed, which means that its composition is uniform throughout the specific indoor environment under study.”
One parameter studied by the researchers was how mask wearing affected the probability of COVID-19 infection. Peng says, “We looked at two factors in evaluating masks, which are the exhalation filtration efficiency and the inhalation filtration efficiency. In all our evaluations, we studied individuals with no masks, surgical masks and N95 respirators. The excess carbon dioxide level that may lead to a certain level of infection risk is 30 times higher for individuals wearing N95 respirators than surgical masks. But the excess carbon dioxide level is two times lower than for individuals wearing no masks.”
The first series of studies that were done involved educational activities. Peng says, “We focused on education because many individuals are thinking about it, particularly with the concerns about reopening schools around the U.S. In doing our evaluation, we analyzed the room volume, occupancy and ventilation rate of a classroom on the campus of the University of Colorado.”
In the case of a classroom lecture, the tolerable excess carbon dioxide level, if the instructor is infected, is approximately 1.5 order of magnitude lower than if a student was infected because the instructor is vocalizing, which will lead to greater virus exhalation than the students. But if a physical education class occurs in the same indoor environment, the excess carbon dioxide level is much lower than for the infected student in a lecture because greater inhalation is occurring due to exercise.
Other cases studied included a COVID-19 superspreader event involving a choir, a subway car operating in a major North American city, a grocery store located near the University of Colorado and a sports stadium located in Germany.
In every scenario, the researchers evaluated a list of parameters to determine which ones will most influence the risk of COVID-19 infection. Peng says, “We determined that physical activity intensity and vocalization level are the two most important parameters that can lead to an increased risk of becoming infected with COVID-19. While vocalization may not affect carbon dioxide exhalation to a large extent, it may facilitate the release of hundreds of times more virus-containing aerosols from an infected person than if the individual was not speaking.”
Future work will focus on development of a simple indicator to evaluate the risk of infection from COVID-19 and other respiratory diseases through aerosol transmission of viral particles. Peng says, “We are working to combine all of the factors studied that impact infection risk into a single indicator.”
The researchers feel that using their full model to calculate the value of absolute infection risk may be difficult. They believe that minimizing the level of excess carbon dioxide in an indoor environment through reducing physical activity and vocalization to as low a level as practical should reduce the relative risk of infection from COVID-19 in a specific inhibitor environment.
Additional information on this research can be found in a recent article
2 or by contacting Peng at
zhe.peng@colorado.edu.
REFERENCES
1.
Howell, J., Passman, F., Woods, B. and Canter, N. (2020), “How to remain safe and productive in working with metalworking fluids during the COVID-19 pandemic,” TLT,
76 (10), pp. 26-36. Available
here.
2.
Peng, Z. and Jimenez, J. (2021), “Exhaled CO
2 as a COVID-19 infection risk proxy for different indoor environments and activities,”
Environmental Science & Technology Letters,
8 (5), pp. 392-397.