How to remain safe and productive in working with metalworking fluids during the COVID-19 pandemic
John Howell, Dr. Fred Passman, Bill Woods and Dr. Neil Canter | TLT Webinars October 2020
A better understanding of how the virus is transmitted, industrial hygiene and how to use disinfectants is essential to stay safe and productive.

KEY CONCEPTS
• The virus causing COVID-19, SARS-CoV-2, can infect individuals through inhaling or ingesting virus droplets present in the air or by contacting droplets on surfaces.
• Industrial hygiene techniques implemented through the use of engineering controls, work practice controls and administrative controls are needed to minimize exposure to SARS-CoV-2 in an end-user’s facility.
• Proper use of disinfectants minimizes the risk of contracting SARS-CoV-2 from touching hard surfaces. One area to prioritize when using disinfectants in the workplace is bathrooms.
This article is based on an STLE Webinar presented to provide assistance to STLE members trying to deal with the COVID-19 pandemic. The origin of the webinar goes back to early March 2020 when the extent of this health crisis became evident in much of the world.
The presenters of this webinar (and authors of this article) started to receive questions about the virus that causes COVID-19, SARS-CoV-2, from individuals working in the metalworking fluid industry. Concern was expressed about whether an individual can be infected working with metalworking fluids.
There are still a lot of questions about SARS-CoV-2 since the virus has only been known for about one year. The purpose of the webinar and this article is to assist those working in the tribology and lubrication field with navigating through the pandemic, keeping safe and being productive.
This article is organized in a similar manner to the webinar into the following four sections:
• STLE Fellow Dr. Fred Passman, principal of BCA in Princeton, N.J., discusses SARS-CoV-2, the symptoms of COVID-19 and how people become infected.
• STLE Fellow Dr. John Howell, principal of GHS Resources in Edinboro, Pa., covers how to remain safe at this time through practicing industrial hygiene.
• Bill Woods, technical marketing and training manager for Pilot Chemical in West Chester, Ohio, discusses the basics of disinfectants, which have become a very important tool used to deal with COVID-19. The subjects of disinfectant claims, labels and how to use these materials are covered.
• Quest ions from the webinar’s Q&A sessions are documented and answers provided.
Understanding COVID-19
An image of the SARS-CoV-2 virus is shown in Figure 1 along with the structure of its key components. Passman says, “SARS-CoV-2 is known as a coronavirus because the protein spikes (see the left image in Figure 1) that are present on the outside are analogous to solar flares from the corona around the sun.”
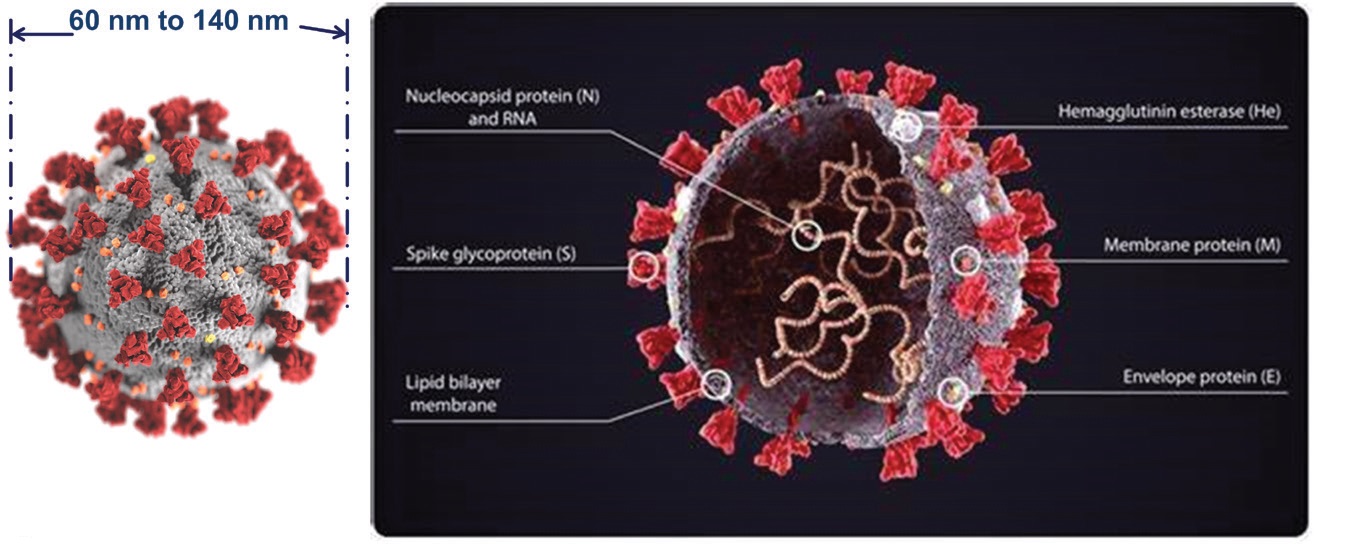
Figure 1. The size and composition of a SARS-CoV-2 virus particle is shown. Figure courtesy of BCA.
Passman indicates that SARS-CoV-2 has a relatively complex structure with the key genetic material in the interior composed of ribonucleic acid (RNA). He says, “The lipid bilayer membrane and the membrane protein are important features because they protect the RNA and enable the virus to be persistent outside of host cells.”
This virus is a member of a class of viruses, several of which have been identified as causing the common cold. Another consequential member of this virus class caused the SARS outbreak of 2013. SARS is an acronym that stands for severe acute respiratory syndrome.
In a similar manner to other viruses, each particle of SARS-CoV-2 is between 60 and 140 nanometers in diameter, which is one to two order of magnitudes smaller than the size of bacteria (generally in the 1-5 micron range). Passman says, “The issue of particle size is particularly important because as the size of a particle decreases, the potential distance it can travel increases (see Figure 2). Viruses are equivalent in size to vapor that can remain suspended in the air for a long period of time. Without rapid air replacement, virus particles might remain in the environment for hours, increasing the chances of transmission and, as a consequence, infection.”
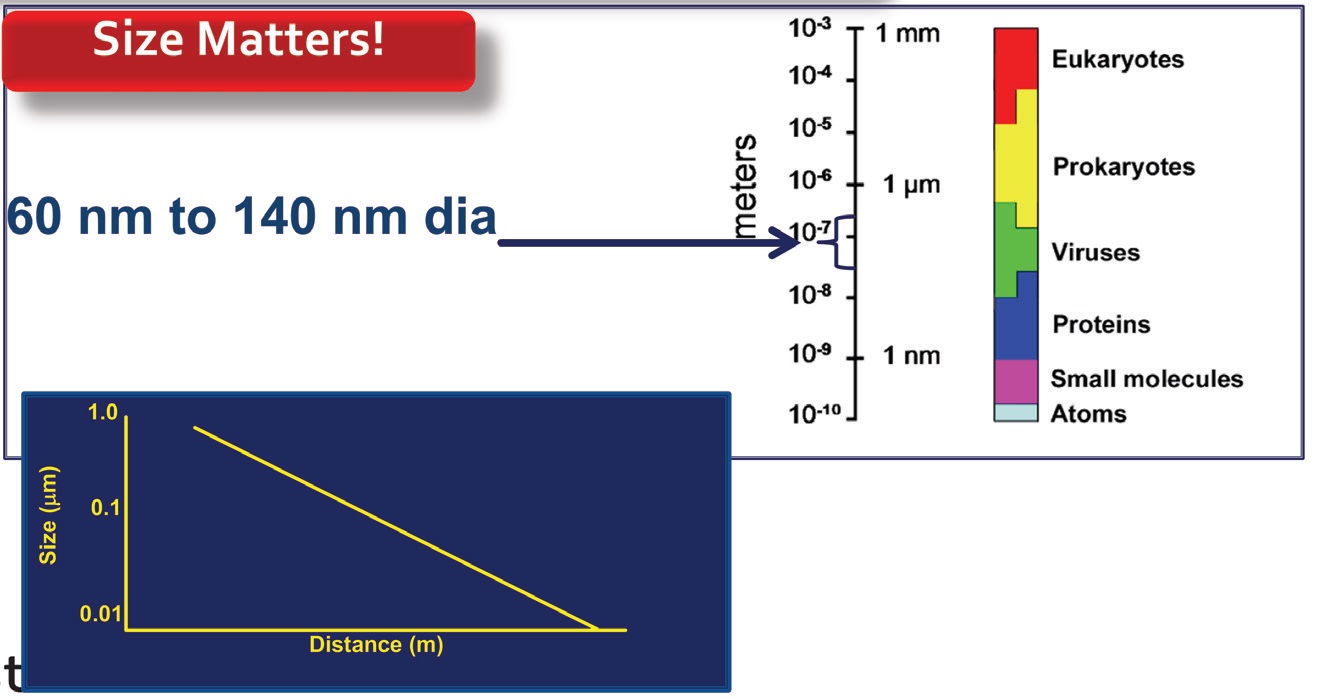
Figure 2. The smaller size of virus particles is an important factor in causing transmission from one individual to another. Smaller particles have a better chance of traveling longer distances than larger ones. Figure courtesy of BCA.
The three most common symptoms of COVID-19 are fever, coughing and fatigue. Passman says, “Fevers can range as high as 104 degrees. Coughing occurs because the virus can cause plaque on the walls of alveoli, thereby creating congestion. The resulting decrease in oxygen exchange in the lungs leads to fatigue and depletion of blood oxygen concentrations.”
Other symptoms include general breathing problems, muscle aches, chills, a sore throat, headache and chest pain.
Passman then explains the infection cycle that details how people can become afflicted with SARS-CoV-2. He says, “It starts with the specific germ and continues with individuals and animals that act as sources (reservoirs) for the germs. Of consequence is that the germ reservoirs can act as carriers even when they are symptom free. The next phase of the cycle is introducing the germ into the environment most typically through the mouth by speaking, sneezing or coughing. This leads to how a new individual becomes infected either through inhaling or ingesting virus droplets or by contacting droplets on surfaces. In the latter case, an individual touches a contaminated surface and then brings their hand to their mouth, nose or eye providing an avenue for the virus to enter a new host.”
Passman points out that it is not entirely clear whether the mode of transmission is through inhalation, ingestion or a combination of both. He says, “Larger particles that are ingested through the mouth might move into the lungs due to the action of the epiglottis (a check valve) that regulates what enters the body’s respiratory and digestive systems.”
Passman draws an analogy regarding virus transmission to the movement of metalworking fluid mist around an end-user’s facility (see the top left image of Figure 3). He says, “High velocity flooding of metalworking fluid impacts the interphase between the cutting tool and the workpiece generating a large quantity of aerosols. Larger (>10 micron diameter) aerosol droplets fall out of the air within a meter from the mist generation source, while the smaller ones form mist and can remain in the environment of the metalworking fluid facility for a longer period of time.”

Figure 3. Aerosols containing the SARS-CoV-2 virus can be transported around an end-user’s facility in a similar manner to metalworking fluid mist. Figure courtesy of BCA.
Passman indicates metalworking fluid mist was more of an issue prior to the wider use by end-users of machine enclosures. The image of particles produced during a sneeze (see bottom left image of Figure 3) shows how the larger ones drop readily out of the air while the smaller ones remain in the environment.
Surfaces present in both small and large machine shops are possibly sources of infection. As shown in the right image of Figure 3, the enclosed machines present in many large machine shops still have surfaces that can be the source of COVID-19 infection. The middle image of Figure 3 shows a location where an employee is making a cup of coffee. Passman contends that coffee left out in the environment can be a source of virus particles that are transmitted by ingestion.
The last step of the infection cycle is the transmission phase to the next individual. Passman states it is not entirely clear why susceptibility to and severity of the disease varies so much among individuals. Among individuals exposed to the same number of viruses, responses range from some remain asymptomatic as others develop fatal infections. He says, “We do not know the magic number of viruses that an individual must either inhale or ingest that will guarantee infection.”
The virus entering the body does not guarantee infection, as Passman states that the steps needed to produce any infection also are very complex. He says, “One important point is that plaque in the blood is extremely vulnerable to attack by the virus, leading to lung blockage and to strokes. This phenomenon is more likely to occur with older individuals due to the higher level of plaque they develop over time. These are known as secondary effects that can make it more challenging for clinicians to diagnose COVID-19 as the cause.”
The complexity of the infection process is not just in the body but in the cell. Passman says, “Lots of things have to line up for the body to be infected and for SARS-CoV-2 to be able to replicate itself in a host cell and release more viruses to infect additional cells.”
Passman then discusses communicability—the probability of SARS-CoV-2 virus passing from one individual to another and causing the exposed person to develop COVID-19. Factors involved include the number of infectious particles that an individual encounters. There is a direct correlation between the risk of getting a disease and the number of particles an individual contacts. A second issue is one of virulence, which means how many SARS-CoV-2 particles must be absorbed by a specific individual to create an infection. Passman says, “We know that the higher the number of virus particles that are present in an infected individual, the greater the chance of infection. But uncertainty exists about the number. But is SARS-CoV-2 as infectious as anthrax, where it has been proven one bacterium is all that is needed to produce the disease in a person?”
The probability of disease transmission is summarized in Figure 4. Passman says, “A number of papers have been published that indicate individuals in an early period (up to five days) before showing symptoms can be highly contagious. This means that COVID-19 might be transmitted just through breathing and talking.”
Noteworthy in Figure 4 is that the number of virus particles peaks as an individual is still symptomatic. As an individual’s immune system successfully deals with the virus, the number of particles steadily declines, leading to convalescence and reducing the risk of the individual transmitting the disease to other people.
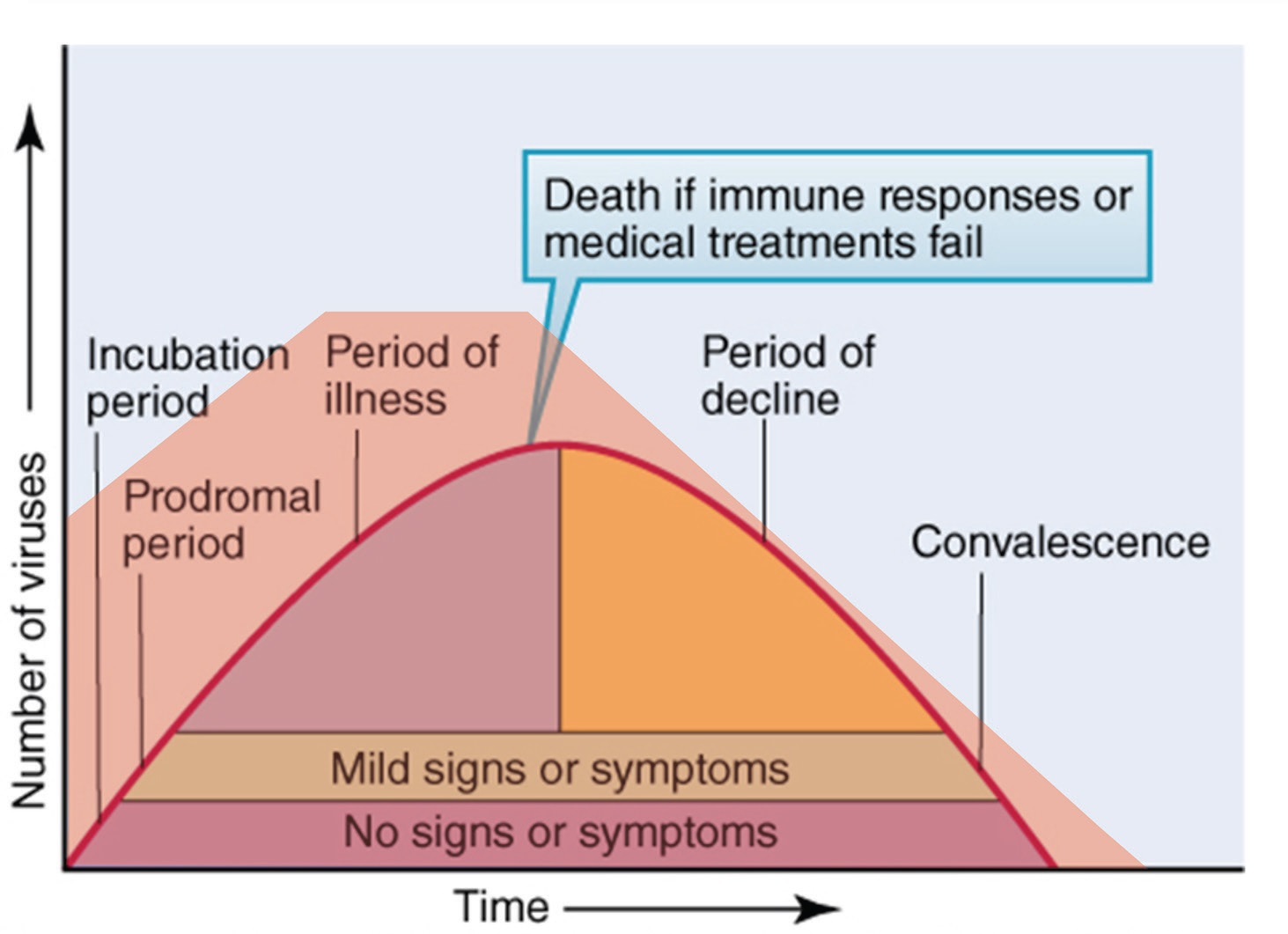
Figure 4. The time progression for an individual exposed to COVID-19 is shown. Of most concern is that an individual might be most contagious before showing symptoms. Figure courtesy of BCA.
The final aspect of assessing the COVID-19 pandemic is to investigate how extensively the disease is impacting the human population. Passman terms this as the study of disease incidence or epidemiology.
To accomplish this task, data needs to be collected, and Passman warns that if this is not done properly, then the results will be misleading. He says, “Statistical analysis needs to be done, but the problem is that some of the test methods used and the results produced have been unreliable. One other issue is the test kits in use are not readily available. Moreover, the number of individuals tested also is not representative of the general population, which means that the data produces misleading conclusions. Only 20% of the U.S. population has been tested to date.” Insufficient and unreliable input data lead to questionable statistics. Moreover, statistics reporting tends to be overly simplified. Passman stated that he has discussed the oversimplification issue elsewhere.
The data collected by epidemiologists is used in the development of models to assist with helping to prevent the spread of the disease. Risk factors (such as age, overall health, pre-existing conditions and prolonged exposure) are analyzed by various organizations (such as the World Health Organization) that provide guidance on managing the risk of contracting COVID-19.
Industrial hygiene
Howell introduces the concept of industrial hygiene and how it can be applied to assist individuals with remaining safe during the COVID-19 pandemic. Besides covering industrial hygiene basics, Howell emphasized that other outside resources are available to assist individuals and their organizations. He says, “You do not have to deal with COVID-19 alone.”
Howell defines industrial hygiene as the science of anticipating, recognizing, evaluating and controlling workplace conditions that might cause workers injury or illness. The intimate contact metalworking fluids have with workers in end-user facilities has led to industrial hygiene being used extensively to assist with such functions as helping to understand the effect of a specific additive. Howell says, “The same basic concepts also apply to the current situation where the metalworking fluid industry is trying to get a better handle on how SARS-CoV-2 is transmitted and what steps need to be done to reduce the chances of infection.”
A good reference for information on industrial hygiene can be found in OSHA Publication 3143 that was initially published in 1998 but has been revised.1 Industrial hygienists use a combination of environmental monitoring and analytical methods.
A hierarchy is present for industrial hygienists to use in dealing with a problem. As shown in Figure 5, Howell indicates that engineering controls are evaluated, followed by work practice controls and administrative controls.

Figure 5. Industrial hygienists (IHs) follow a hierarchy starting with engineering controls in dealing with a problem. Figure courtesy of GHS Resources.
Engineering controls have been used to eliminate toxic chemicals in an end-user’s facility or replace harmful materials with less hazardous ones. Howell says, “Concern about COVID-19 has increased the importance of enclosing work processes (such as machine tools) and installing and maintaining general and local ventilation systems. These approaches have proven to be useful in the past in minimizing worker exposure to metalworking fluids. Now, they can be applied from a COVID-19 standpoint to ensure the air in the end-user facility is well maintained. After all, a contagious worker with a cough can spread virus particles quite a distance, which might lead to transmission if there is inadequate ventilation.”
In moving to workplace controls, past efforts to minimize worker exposure to metalworking fluids have been successful. Howell says, “Now, the situation has changed as procedures need to be developed to minimize worker-to-worker interactions through the practice of social distancing.”
Among the techniques that industrial hygienists need to stress is the implementation of good housekeeping procedures. Howell says, “What we used to do in end-user facilities years ago and even months ago is not good enough. There is a real need for good housekeeping today during the COVID-19 pandemic.”
Managers working in end-user facilities need to practice industrial hygiene by conducting good supervision. Howell says, “They need to take time to walk around the facility and see what their employees are doing rather than hiding in their offices.”
One other aspect of workplace controls is to make sure workers understand that taking breaks to eat, drink, smoke, etc., in restricted workplace environments cannot be tolerated because they can lead, inadvertently, to transmission of the virus.
The main objective of administrative controls is to work with employees to minimize exposure and maximize productivity, not just to metalworking fluids but to each other. Howell indicates measures such as scheduling production and worker’s tasks properly are necessary to achieve this objective. In addition, personal protective equipment (PPE) must be tailored to each worker. For those who have particular sensitivities and might be high risk, additional measures such as face shields and N-95 respirators might be advisable.
These measures can be critical as Howell points out, because individuals who transmit the SARS-CoV-2 virus in many cases can be asymptomatic.
From an outside resource perspective, the first place recommended by Howell to turn is a link to “what is new regarding COVID-19” on the CDC website.2 He says, “Information on COVID-19 covering the key industrial hygiene practices gets updated almost daily. CDC provides guidance on how to do daily health checks, find locations with the highest risk of exposure, deal with making sure workers are properly protected by using face coverings, how to make sure employees practice social distancing and improving the facility’s ventilation system.” Howell encourages everyone to bookmark this page.
Among the challenges is convincing employees that wearing face coverings is effective and will help to reduce transmission of the virus. Social distancing must be done not only in the plant but also in areas such as the cafeteria where employees tend to congregate. Improving ventilation can be easier in the summer with open windows facilitating rapid turns of air. But this can become more of a challenge in the winter when it is harder to circulate fresh air.
Howell points out that a second very useful CDC document is the “Resuming Business Toolkit”3 that was published in the spring of 2020. Among the concepts covered are encouraging sick employees to stay home, daily health checks whether in-person or virtual and establishment of a COVID-19 coordinator and a cross-functional team onsite at the workplace. He adds, “Every workplace needs a COVID-19 coordinator to evaluate how work is being done, how employees are interacting with each other and to make sure that every department is following the same approach to minimize transmission of the virus.”
Complementing CDC is OSHA, which has done a good job of providing new information on COVID-19, according to Howell. He says, “A good reference is OSHA 3990-034 that provides guidance on returning to work and was published in March 2020. Among the key pointers is how to identify sick employees before they enter the workplace and infect others.”
The National Association of Manufacturing also has documents5 that can help metalworking fluid and lubricant producers rethink their processing from a health and safety perspective utilizing technology. Among its input is a report from its leadership council that urges manufacturers to consider new operational practices.6
Other resources are available through ILMA7and from STLE.8 In the latter case, an article from the July 2020 issue of TLT discusses how COVID-19 is impacting the global lubricant industry.
Howell concludes, “If you are in a position to employ industrial hygiene techniques, the more you know about what you are trying to do and the more you are familiar with the outside resources discussed, the better you will be able to advise your own company or make recommendations in your own facility about what to do. It will come down to using the basics of industrial hygiene to instill the key concepts required to minimize the chances of individuals becoming infected with SARS-CoV-2.”
Disinfectants
The focus of the discussion on disinfectants is to minimize the risk of becoming infected from touching hard surfaces where other individuals who had contracted COVID-19 might be living and working. Woods says, “To reduce the risk of infection, there are tools available that can be used to treat surfaces.”
Woods points out that those tools are known as disinfectants, which are regulated in the U.S. by EPA under the Federal Insecticide, Fungicide and Rodenticide Act (FIFRA). He says, “EPA defines disinfectants as pesticides due to their effectiveness in eliminating a pest such as bacteria, fungi or viruses. The chief means for regulating chemicals used in disinfectants is registration. In this process, EPA has strict requirements governing product labels, which is their key approach for ensuring the safe use of disinfectants. Suppliers of disinfectants consider the label to be the law.”
Use of disinfectants is enforced on the local and state level through a combination of civil and criminal penalties.
The label is one of three components that make up a disinfectant. Woods says, “The second component is the recipe, which EPA considers the confidential statement of formula (CSF). Besides the active ingredient that is responsible for supporting the antimicrobial claims of the disinfectant, inert ingredients such as water, dyes, perfume, chelating agents and detergents also can be present. The third component is data, which is generated to demonstrate that the active ingredient will, in fact, kill a specific pathogen such as SARS-CoV-2. Every antimicrobial claim made by a disinfectant supplier must be supported by data produced through extensive testing. This data supports claims made by the disinfectant supplier and represents the major development cost.”
Woods maintains that a recipe can only be approved as a disinfectant by EPA if it meets specific testing criteria. A disinfectant must either completely eliminate 100% of a specific microbe or else achieve a six-log reduction in the microbe’s concentration on a surface. This applies to disinfectants designed to eliminate specific pathogens such as SARS-CoV-2.
This criteria applies no matter if the disinfectant is a virucide that targets a specific virus or a fungicide that eliminates 100% of a specific mold. Woods says, “Testing of viruses is particularly challenging because this parasitic microbe is technically not a living organism and must be grown through culturing.”
Woods also draws a distinction between removal of a specific microbe and sterilization. He says, “Elimination of a specific microbe does not mean that a specific surface has been sterilized through removal of all living organisms but only indicates that the targeted microbe has been removed.”
Though not covered in detail in this webinar, sanitizers have now also gained in popularity as a way to reduce the possibility of infection. These materials also are regulated in a similar manner by EPA. Woods says, “Two classes of sanitizers are designed for treating non-food contact and food contact surfaces. In the former case, the sanitizer must eliminate 99.9% or a three-log reduction of the targeted microbe. For the latter, the sanitizer must eliminate 99.999% or a five-log reduction.”
A disinfectant label such as the generic one shown in Figure 6 must provide information on using the specific product. Woods says, “The label identifies the brand name, documents the specific antimicrobial claims, provides specific directions for use and has a precautionary statement. The identity of the active ingredient is shared along with directions on storage and disposal. One important issue to consider is whether the disinfectant is allowed to be used on surfaces that touch food.”

Figure 6. A generic label for a disinfectant is shown. Figure courtesy of Pilot Chemical Co.
Woods emphasized that the safety information on a disinfectant label should be reviewed very carefully to determine what PPE is required during use. He says, “Check to make sure that goggles and/or gloves might be needed when working with the disinfectant. Also, since the disinfectant is a pesticide, it should be kept out of the reach of children.”
In reviewing the disinfectant label, Woods indicates that the EPA registration number (shown on the bottom left of the label) is of value in determining whether a specific product is effective on a particular pathogen. Woods says, “An example of an EPA registration number is shown in Figure 7. Often a user will see either two sets or three sets of numbers. The first series of numbers identifies the company that developed the disinfectant and registered it with EPA. Each disinfectant formula is assigned a specific number by EPA. The final four numbers identify the company that sub-registers the disinfectant in order to act as a distributor. This is the organization that actually sells the product. Not every company that develops a disinfectant will actually sell the product.”

Figure 7. Every disinfectant sold in the U.S. has a registration number that contains a company number, formulation number and distributor number. Figure courtesy of Pilot Chemical Co.
To find a disinfectant that works on a particular pathogen, EPA has prepared and published 15 lists that inform the user about which disinfectants are effective against specific pathogens. Those products on each list have been tested to verify they are effective against the designated pathogen.
Woods says, “For newly identified pathogens, EPA implements an emerging pathogen program. Such a program was activated to deal with SARS-CoV-2 in January 2020. List N was initiated by EPA and can be found on the organization’s website.9 For new viruses, EPA will evaluate the efficacy of disinfectants on similar pathogens and those that are more resistant. All disinfectants on List N meet EPA’s criteria for dealing with the virus that causes COVID-19. They have either demonstrated efficacy against SARSCoV-2, a more resistant virus or another type of coronavirus that is similar.”
EPA has classified SARS-CoV-2 as an EPP class III, enveloped virus, which is the least resistant to chemical disinfectants. Woods adds, “Testing against SARS-CoV-2 just began in April 2020. A few disinfectants have recently been tested and found to be effective against this virus. Many more disinfectants are undergoing testing, and EPA is expected to indicate they are effective against SARS-CoV-2 by the end of 2020. Currently, over 400 disinfectants are on EPA List N. Users are encouraged to review List N to confirm that the disinfectant of choice is effective.”
When applying disinfectants, Woods urges the user to follow directions, use recommended PPE, apply the disinfectant in the recommended manner and be aware of having adequate ventilation. He says, “Only apply to those surfaces (such as floors, walls, etc.) identified on the label. Allow the disinfectant to wet the surface for the dwell time listed on the label. A standard dwell time is about 10 minutes.”
Areas to prioritize in the workplace are shown in Figure 8. Woods says, “In my experience, bathrooms are a particular hot spot because they represent another way for the virus to be transmitted. They deserve special attention along with kitchens in workplaces because people tend to congregate in these places, leading to easy transmission of the virus.”

Figure 8. A particular hot spot where the SARS-CoV-2 virus can be transmitted is the bathroom. Figure courtesy of Pilot Chemical Co.
A summary of the “dos” and “don’ts” in using disinfectants is shown in Figure 9. Of particular importance is users should not mix disinfectants with anything besides water. While adding disinfectants to cleaners might be tempting, the two product types are incompatible, and the cleaner will nullify the effectiveness of the disinfectant.

Figure 9. (Left) General guidelines are shown for how to properly apply a disinfectant and (right) what should not be done in working with a disinfectant. Figure courtesy of Pilot Chemical Co.
Q&A
CDC and other organizations now indicate that the main source of COVID-19 transmissions is through the air in a person-to-person manner. They claim there is less concern about contracting the virus from surface transmission. What is the viewpoint of the panelists?
Passman: Just recently, new research papers have been published that question the value of surface disinfection in places such as public transportation (buses, trains, etc.). In this particular application, equipment used has now been taken out of service for several hours each day to be thoroughly cleaned with certified disinfectants. The major way for transmission to take place through surface contact is for an individual to then touch their face. Use of masks appears to be very helpful in this regard by discouraging individuals from touching their faces. But there is still a chance for transmission to take place by touching surfaces because the virus can remain active on a specific surface for some time depending upon the type of surface and the environment. With that said, the CDC and other organizations are correct in that people trapped in closed spaces for long periods of time are at the greatest risk through person-to-person transmission.
Howell: While picking up the virus from a surface could be an issue, Woods has explained that proper use of disinfectants should minimize that risk. The focus should be on minimizing person-to-person transmission in facilities such as plants through social distancing and preventing those individuals who do not feel well from entering the specific facility.
Woods: Disinfecting surfaces is still important and should be done by prioritizing specific areas such as bathrooms where there is a greater chance of transmission from urine and sweat.
Would you expect a typical alkaline metalworking fluid to spread COVID-19?
Passman: Viruses are not likely to persist for a long period of time in alkaline metalworking fluids. But there is no data to verify this, so it is impossible to say no! Hopefully data will be generated in the future to confirm this answer.
STLE Fellow Neil Canter, principal of Chemical Solutions in Willow Grove, Pa., says, “Many of the alkaline metalworking fluids are emulsions whether they be emulsifiable oils or semisynthetic fluids. Both fluid types contain emulsifiers that tend to inactivate viruses such as SARSCoV-2 in a similar manner to common soap. The hydrophobic component (or tail) of an emulsifier can break open the lipid bilayer membrane of the virus (see Figure 1) inactivating the virus particle. The hydrophilic component (head) of the emulsifier will lift the virus off of a surface (including hands) allowing it to be washed away. This is why all of us are encouraged to frequently wash our hands with soap.”
What information is available about whether the common metalworking fluid biocides (such as HHT) have any effectiveness toward SARS-CoV-2?
Passman: Many of the common biocides such as HHT and isothiazolinones are not used to disinfect surfaces, which means there is uncertainty about their effectiveness toward SARS-CoV-2. HHT and other formaldehyde-releasing biocides denature the virus membrane, which increases their chances of inactivating SARS-CoV-2. Isothiazolinones are probably not effective because they primarily target the energy metabolism pathway of microbes. Viruses are not alive and do not have this type of pathway. Some hindered phenolics are on EPA’s List N and considered to be effective against COVID-19. But a user needs to check the specific composition of the phenolic to make sure it has been approved for use against SARS-CoV-2.
Woods: No data is available to indicate that metalworking fluid biocides are effective against SARS-CoV-2.
Does having COVID-19 give an individual immunity in the future?
Howell: It is impossible to speculate on this question because the data is still under development at this time.
Passman: The antibody count of people who recover from COVID-19 seems to go down quickly over time. But what is not known is how quickly this occurs. The body’s immune system is quite complex, so there is a chance that cells are present that remember SARS-CoV-2 and can activate the immune system if this pathogen re-enters a specific individual in the future. Nobody knows what types of symptoms individuals who are infected more than once will show. Obtaining data to answer this question could be challenging because individuals who contracted COVID-19 once might be more cautious and might tend to remain in seclusion.
Can an individual contract COVID-19 again?
Passman: No data is available to indicate whether an individual has immunity or can contract COVID-19 again.
STLE encourages continuing interaction with its membership on the challenges faced in dealing with COVID-19. Members are encouraged to submit questions and comments to STLE at information@stle.org.
Note: The COVID-19 webinar is available for review on the STLE website here.
REFERENCES
1. Click here.
2. Click here.
3. Click here.
4. Click here.
5. Click here.
6. Click here.
7. Click here.
8. Moncrieff, I. and Phadke, M. (2020), “The impact of the COVID-19 pandemic on the global lubricants industry,” TLT, 76 (7), pp. 34-36. Available here.
9. Click here.
Dr. John Howell has more than 50 years of experience in metal finishing and metalworking R&D, R&D management and chemical health, safety and environmental management. Currently, Dr. Howell is president of GHS Resources, Inc., and he prepares GHS compliant SDSs and consults with clients and trade associations to improve their environmental and health and safety performance. Dr. Howell is an STLE Fellow and a long-time member of ASTM and the American Chemical Society.
Dr. Fred Passman is an ASTM Fellow, STLE Fellow and Certified Metalworking Fluids Specialist, with more than 45 years of experience in environmental-industrial microbiology. He is the principal of Biodeterioration Control Associates. Since 1973, Dr. Passman has conducted research and consulted to government and private industry on topics as diverse as composting municipal sewage sludge, U.S. EPA criteria for various groups of toxic substances in fresh-water systems, microbially enhanced oil recovery and microbial contamination control in industrial process fluids. Dr. Passman is a member of numerous professional and trade organizations including ASTM, the International Biodegradation & Biodeterioration Society and STLE.
Bill Woods provides marketing support for the Pilot Chemical Co. antimicrobial products sold through the Mason Chemical business unit. Woods’ responsibilities include identifying new opportunities for Pilot Chemical Co. antimicrobials, monitoring new trends in disinfection and training their sales managers. Woods has more than 30 years of experience in various commercial and technical capacities including sales, marketing, technical service and product development at Arch Chemicals, CasChem, Galaxy Surfactants and Lonza. He has a master’s of business administration in marketing, master’s of arts degree in science and bachelor’s of arts degree in chemistry/biology.
Dr. Neil Canter is an STLE Fellow and a Certified Metalworking Fluids Specialist, with more than 35 years of experience in working with metalworking fluids. He is the principal of Chemical Solutions. Dr. Canter has a strong background in the chemistry of metalworking fluids and in regulations impacting their use. He is a member of the American Chemical Society, the Society of Automotive Engineers, STLE and a contributing editor to TLT.